Epidemiology of multiple sclerosis
Epidemiology is the branch of medicine that studies the frequency and pattern of a disease as well as the causes and risk factors in specific populations, according to “A Dictionary of Epidemiology.” The scientists who work in this field are called epidemiologists.
While MS is not contagious nor directly inherited, epidemiologists have identified factors involved in the distribution of MS around the world. These factors include sex, genetics, age, geography and ethnic background. Understanding what causes MS will help us find more effective ways to treat it and — ultimately — cure it, or even prevent it from occurring in the first place.
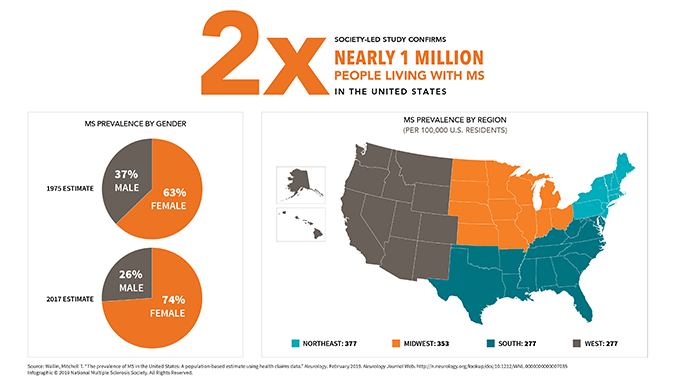
A 2019 study confirmed that nearly 1 million people are living with MS in the U.S., more than twice the previous estimate.
At what age is MS usually diagnosed?
Most people are diagnosed between the ages of 20 and 50, although MS can occur in young children and older adults.
Where is MS most common geographically?
In general, MS is more common in areas farthest from the equator. However, prevalence rates may differ significantly among groups living in the same geographic area regardless of distance from the equator.
The role of sex hormones in multiple sclerosis
The recent prevalence study shows that MS is 3 times more common in those assigned female at birth than male. This suggests that hormones may also play a significant role in determining susceptibility to MS.
Does ethnic background affect who gets MS?
Research has demonstrated that MS occurs in most ethnic groups, including African Americans, Asian Americans and Hispanics/Latinx in the U.S., but is most common among white people of northern European descent. Susceptibility rates vary among these groups, with recent findings suggesting that African American women have a higher than previously reported risk of developing MS.
What is the genetic risk of MS?
MS is not an inherited disease, meaning it is not a disease that is passed down from generation to generation. About 200 genes have been identified that each contribute a small amount to the overall risk of developing MS. In the general population, the risk is about 1 in 333.
What are other risk factors for MS?
Evidence shows that low vitamin D levels, smoking and obesity all play important roles in the development of MS. Many viruses and bacteria have been or are being investigated in connection with MS as well. A growing number of research findings indicate that previous infection with Epstein-Barr Virus (EBV), the virus that causes mononucleosis, contributes to the risk of developing MS.
Learn more about the possible causes of MS.
Epidemiological estimates
Although more people are being diagnosed with MS today than in the past, the reasons for this are not clear. Likely contributors include greater awareness of the disease, better access to medical care and improved diagnostic capabilities. There is no definitive evidence that the rate of MS is generally on the increase.